Life in Motion Program
If you’ve been living with persistent pain for months or years, especially if scans are normal and treatments haven’t helped, the Life in Motion program offers a structured pathway for retraining the nervous system and restoring trust in your body.
Life in Motion is a structured, three-phase program for people living with chronic primary pain (also called neuroplastic pain). It integrates Pain Reprocessing Therapy (PRT) with osteopathic manual therapy to help the nervous system unlearn persistent pain patterns and rebuild confidence in movement and daily life. Pain Reprocessing Therapy is a behavioural neuroscience-based approach supported by emerging research in pain science and behavioural medicine.
This is not open-ended, visit-by-visit care. Life in Motion provides a clear clinical pathway: assessment and education, skill development and real-life application, followed by long-term maintenance and relapse prevention.
A 6-Month Structured Pain Reprocessing Therapy Program (12 Sessions)
The Life in Motion Pathway Overview
The Life in Motion pathway is structured and progressive. Below is a visual overview of how care unfolds.
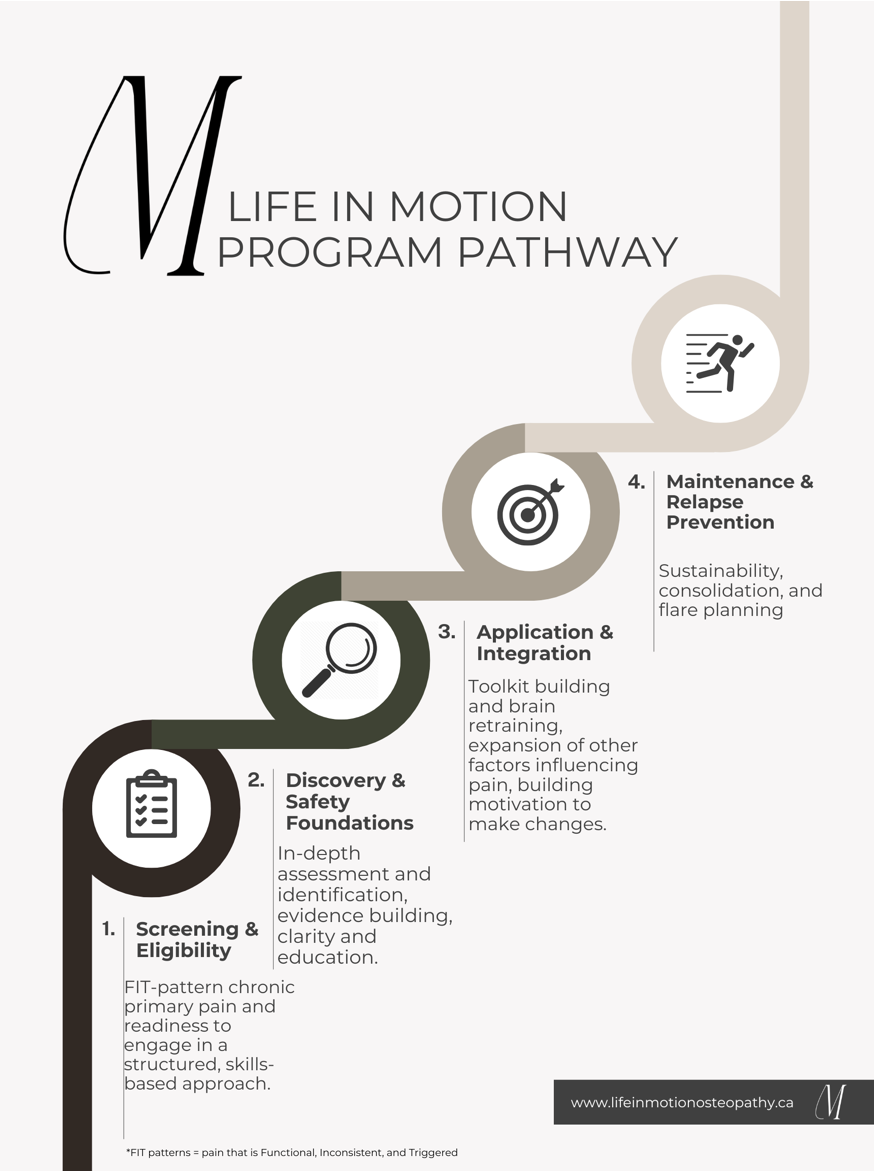
FIT patterns refer to pain that is Functional, Inconsistent, and Triggered. Eligibility is confirmed during the screening call.
Phase 1 — Discovery & Safety Foundations
Sessions 1–4 | Weekly
Phase 1 focuses on building understanding and safety. We begin with a comprehensive intake and physical assessment to ensure we’re working from a clear clinical picture. From there, we develop a personalized understanding of your pain through the lens of modern pain science and the pain-fear cycle.
You’ll begin gathering your own evidence for how context, attention, stress, and protective patterns influence symptoms. Foundational pain-safety learning and nervous system stabilization strategies are introduced alongside gentle “green-lighted” movement.
Phase 1 supports:
- Reduced fear and uncertainty about pain
- A clearer explanation for why pain persists
- Early reconnection to safe movement and daily activity
- A stable foundation of safety for deeper retraining
Phase 2 — Application, Retraining & Integration
Sessions 5–10 | Biweekly
Phase 2 is where retraining deepens. You’ll learn Pain Reprocessing Therapy techniques to interrupt the pain-fear cycle and help your brain interpret sensations through a lens of safety.
We build and refine a personalized toolkit so you know how to respond during flares, triggering activities, or moments when your nervous system shifts into high alert.
This phase includes graded exposure and somatic tracking, movement re-education, outcome-independence coaching, and skill-building around self-compassion and emotional regulation.
We also address other “danger signals” that may keep the nervous system activated — including global factors (overstimulation, pace, digital input) and internal patterns (pressure, perfectionism, worry, preoccupation, shame, fear of sensation).
A central focus is learning to attend to internal state early — so stress and overload don’t quietly accumulate and spill into symptoms.
Phase 2 supports:
- Increased activity tolerance and confidence
- Reduced symptom preoccupation and urgency
- More flexible responses to sensations and triggers
- Stronger self-regulation skills
- A clearer sense of agency in daily life
Phase 3 — Sustainability & Relapse Prevention
Sessions 11-12 I Monthly
Phase 3 focuses on maintenance and long-term confidence. We normalize fluctuations, introduce relapse and extinction burst education, and create a clear flare plan you can return to when symptoms spike.
You’ll leave with a personalized “back-to-basics” framework to respond to flares with steadiness rather than panic or forcing.
We consolidate skills, identify early warning signs of nervous system overprotection, and clarify how to continue applying these tools independently.
Phase 3 supports:
- A personalized relapse-prevention and flare plan
- Stronger self-efficacy and long-term confidence
- Durable gains in function and quality of life
- A clear transition to independent self-management
What Patients Often Describe
“I feel you have not only worked through my presenting issue, but you’ve taught me how to be more self-reliant and in tune with my body. Rather than fighting it and feeling frustrated, I now meet it with curiosity and I’m open to a range of new responses. My nervous system feels reset. My resilience has returned, my pain has subsided, and my body feels like my own again.”
What the Program Includes
- Initial intake session lasting 75min; 11 follow up sessions lasting 60min
- Integrated manual therapy and guided movement
- Structured education and practical skill-building
- Worksheets and resources to support home practice
Program Investment: $2,450 (including HST)*
*Payment plans available upon request.
Why Six Months?
Six months allows time to build safety, practice new responses in real life, and consolidate change without pressure or urgency. Persistent pain patterns driven by nervous system sensitization do not shift through insight alone — they change through repetition, consistency, and gradual re-engagement with meaningful activity.
Who This Program Is For
Life in Motion may be appropriate if you are experiencing persistent pain lasting longer than three months that continues despite time, treatment, or reassuring imaging — particularly when symptoms fluctuate with stress, attention, or context, or when fear and activity avoidance have become part of the pattern.
This program is designed specifically for chronic primary pain presentations with FIT features (Functional, Inconsistent, and Triggered patterns).
It is not intended for active inflammatory disease, progressive neurological conditions, or untreated structural pathology. Individuals with these concerns are referred appropriately for medical evaluation.
A brief screening call is required to determine clinical fit and readiness to engage in a structured, collaborative, skills-based approach
For Physicians & Referral Partners
Life in Motion serves patients experiencing persistent pain patterns, including chronic primary pain and mixed structural–sensitization presentations. Many individuals present with identifiable structural findings while also demonstrating nervous system sensitization that amplifies and maintains symptoms.
The Life in Motion Program provides a structured, nervous system–informed approach designed to reduce fear-avoidance patterns, decrease central amplification, and improve functional capacity. It does not replace medical management. Structural, inflammatory, or progressive conditions are referred or co-managed appropriately.
Physician referral inquiries and collaborative care discussions are welcome. Please contact the clinic directly or use the form below to discuss clinical suitability or coordination of care.
Important Note on Fit and Safety
Participation in the Life in Motion Program begins with a structured screening process to confirm clinical suitability. Eligibility is determined through assessment of symptom history, presentation patterns, and FIT features (Functional, Inconsistent, Triggered pain patterns) associated with chronic primary pain.
This program does not replace primary medical care. It is designed to complement ongoing medical management when appropriate, and collaboration with referring physicians or healthcare providers is welcomed.
If at any point symptoms suggest the need for further medical evaluation or specialist care, appropriate referrals are made.